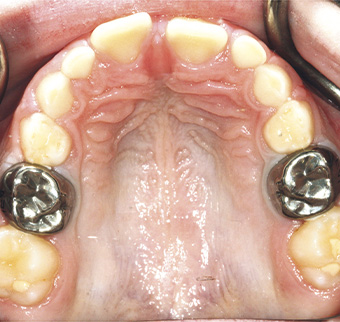
Achieving full coverage
Evelina Kratunova, BDentSc, MFD(RCSI), DCh Dent, FFD(RCSI), and Anne C O’Connell, BA, BDentSc, MS, describe how to achieve full coronal coverage in primary molar restorations
Numerous clinical situations require full coronal coverage in primary molars in order to provide the most durable restoration. Primary teeth with proximal lesions or extensive caries are best managed when restored with crowns. Clinical research has repeatedly confirmed that the success of pulpally treated primary molars significantly depends on an optimal coronal seal of the tooth from the oral environment.
Primary molars with indirect pulp therapy, pulpotomy and pulpectomy procedures have better clinical outcomes when provided with full coronal coverage. Protection of the dentinal-pulpal complex from contamination of the oral environment will promote healing and maintenance of the vitality of reversibly inflamed pulp. Crowns are also indicated for fractured primary molars; developmental defects of the tooth structure; teeth with extensive tooth surface loss due to attrition, abrasion, or erosion; and infra-occluded primary molars to maintain mesio-distal space (Kindelan et al. 2008; Hickel et al. 2005; Randall 2002).
Classification of full coronal coverage restorations for primary molars
Stainless steel crowns (SSCs) are widely recognised for their strength and longevity; however, due to the metallic colour, they lack aesthetics (Randall 2002; Hickel et al. 2005; Kindelan et al. 2008). Chair-side techniques for direct veneering and open-facing have been used to achieve a more natural look of the SSCs.
Over the years, alternative tooth- coloured, full-coverage restorations have been tested using different types of dental materials and techniques with varied levels of success. Commercially fabricated preveneered SSCs combine durability and aesthetics (Fuks et al. 1999; Ram et al. 2004; Leith and O’Connell, 2011; Kratunova and O’Connell, 2014; O’Connell et al. 2014). Prefabricated crowns made from composite resin, polycarbonate and zirconia offer tooth-coloured alternatives.
Conventional stainless steel crowns
Stainless steel crowns (SSCs), also known as preformed metal crowns are prefabricated extra-coronal restorations which can be adapted to individual teeth and cemented in place to provide a definitive restoration (Kindelan et. al. 2008). The SSC is a durable, cost-effective, minimally technique sensitive restorative option that offers the advantage of full coronal coverage and accommodates the majority of treatment indications for primary posterior teeth (Seale 2002).
SSCs were popularised as a restorative method for primary molars in the 1950s (Humphrey 1950; Engel 1950). Over time, SSCs have been modified to improve the anatomical form and the alloy composition (9-12 per cent nickel; chromium 12-30 per cent) (Randall 2002).
The contemporary SSCs are pre-trimmed, pre-contoured and crimped and usually need no or minimal adjustment by the operator. Local anaesthesia is necessary for placement of a SSC. The conventional tooth preparation requires 1-1.5mm occlusal reduction and minimal proximal reduction of the primary molar.
The finish line should be a smooth feather edge at or below the gingival margin with no step or shoulder. A snap fit is achieved when the flexible metal margin passes over the buccal bulbous area and fits into the cervical constriction of the molar. SSC margins can be well adapted into the undercut areas with the help of contouring and crimping pliers (Randall 2002). SSCs cannot be used in children with nickel sensitivity.
Hall technique stainless steel crowns
SSCs can provide optimal isolation of the dentinal-pulpal complex from the oral environment resulting in arrest of the carious tissue, and can promote healing and maintenance of the vitality of reversibly inflamed pulp. This more biological approach to treatment of caries is now gaining popularity (Kidd 2004; Ricketts et al. 2006; Thompson et al. 2008).
Placement of an SSC on primary molars without any prior tooth preparation, decay removal, or local anaesthesia is known as the Hall technique, named after Dr Norna Hall who had used this novel method in her clinical practice since the 1980s. This is the practical application of sealing in caries. The indications for Hall crowns are the same as those of conventional SSCs except where teeth have irreversibly inflamed pulps and dental sepsis (Innes et al. 2009, 2011).
Success of the Hall technique relies on correct pulpal diagnosis. There is no need for local anaesthesia as there is no reduction of tooth structure and no caries is removed. The crown is filled with a glass ionomer cement and pushed onto the tooth thereby sealing the caries lesion from the oral environment. Sometimes use of orthodontic separators is advised to allow easier seating Evidence of the clinical success of this technique after five years is very promising yet limited (Innes et al. 2011).
Pre-veneered stainless steel crowns
The increasing demand for a more natural appearance of the clinically restored primary teeth led to the introduction of the commercially produced aesthetic preveneered stainless steel crowns (VSSCs) for paediatric dental patients . The VSSCs were developed to combine the strength and durability of the conventional SSCs with the aesthetically pleasing appearance of the white veneer facing.
Newly available techniques and materials for bonding of resins to metal surfaces have made this possible. Thermoplastic, composite or epoxy resins were used for the white facing. Mechanical retention or a chemical bonding and coating were described as methods of veneer attachment to the stainless steel core (Hosoya et al. 2002). The exact specifications of the attachment, thickness and pattern of the veneer remains proprietary to the individual manufacturer.
However, the makers of the current leading brands VSSCs – Nusmile www.nusmilecrowns.com and Kinder Krowns www.kinderkrowns.com – have disclosed that the veneer is a composite resin material which is attached either through an intermediate bonding agent to the pre-prepared (e.g. alumina blasted) metal surface or is bonded and additionally mechanically retained to a fenestrated stainless steel core in different patterns .
The composite facing material requires adequate thickness for mechanical strength and ability to withstand occlusal masticatory forces. Therefore in the area of the veneer the VCCSs have increased thickness of 1.5 to 2mm, which is substantially more than the thin stainless steel core of 0.2mm. VSSCs require approximately 20 per cent overall tooth reduction which is much greater than conventional SSC crown preparation.
The manufacturers recommend 1.5-2mm occlusal reduction and circumferential reduction of 1.5mm and should have a smooth finish without undercut areas. This reduction will not result in exposure of the pulp and any pulp therapy will be dictated by the extent of caries. The VSSC should fit passively with the finish line approximately 1mm subgingival.
Unlike the conventional SSCs, the VSSCs cannot be crimped in the areas of the facing so that limited crimping is advised only on margins free of composite veneer. Manufacturers also warn that the metal substructure flexes from pressure during crimping, fitting or seating and this could introduce micro-fractures to the facing which subsequently can progress to veneer loss.
Autoclave sterilisation is discouraged due to risk of discolouration of the facing material and only chemical disinfection is recommended for these crowns.
Prefabricated paediatric zirconia crowns
Zirconia is a ceramic material consisting of zirconium dioxide stabilised with yttrium oxide (ZrO2-TZP; 3 mol per cent Y2O3). Since its introduction for dental use over the past two decades, zirconia has become particularly attractive restorative material due to its exceptional properties combining high aesthetic value and excellent mechanical characteristics (Zarone et al. 2010).
Zirconia is insoluble in water, has very high biocompatibility and it has been demonstrated to not enhance bacterial adhesion and growth (Scarano et al. 2004). Other valuable characteristics of zirconia include favourable radio-opacity, low corrosion potential and the highest flexural strength and fracture toughness among all the other ceramics (Guess et al. 2010). These crowns can be used in nickel-sensitive patients.
Prefabricated paediatric zirconia crowns were first manufactured for clinical use in 2007. The solid zirconia construction offers high strength and durability along with superior aesthetics due to realistic anatomy and shade of the crowns . Other promoted advantages of paediatric zirconia crowns include high biocompatibility and thin gingival margins not interfering with gingival health. Contaminated crowns can be autoclaved without risk of colour change or fault of the structural integrity. The tooth preparation technique for the paediatric zirconia crowns is very similar to that of the VSSCs. The occlusal reduction is about 2mm; proximally and circumferentially the primary tooth is reduced 1.5mm with a subgingival margin extension of 2mm. The zirconia crown should have a passive fit without any tension. The tooth preparation is critical as no crimping is possible in the zirconia crowns and adjustment of zirconia is not advised. Each manufacturer of zirconia crowns proposes different anatomical features that will necessitate alteration of the tooth preparation for maximum success.
Potential limitations of these crowns include risk of wear on opposing natural teeth, de-cementation, chipping, and fractures. These crowns are similar in cost to VSSC but more expensive than conventional SSCs. Paediatric zirconia crown kits have been commercially available for only a few years and are gaining clinical acceptance. There are no prospective clinical trials published so far reporting on the performance of zirconia posterior crowns.
The general dental practitioner should be aware of the advances in restorative paediatric dentistry and the newer options to provide aesthetic full coverage restorations for children. The use of Class 2 restorations using composite, compomer, or glass ionomer should be restricted to small proximal lesions in children at low caries risk, or as a temporary solution.
Full coverage restorations should be used when the proximal lesion is extensive and the child is at risk of future decay. The selection of the best full- coverage restorative options for primary molars must be based on the individual case. Additional training and experience will be required if the clinician is to become competent in each technique.
All these options however are valuable as part of the clinicians’ armamentarium providing restorative choice in the contemporary paediatric dental practice.
A full list of references is available on request.